In this article I will tell you about herpes viruses, their types, the most frequent illnesses that they can cause in human being, their treatments, the roads of transmission of human herpes virus and actions you should execute to prevent the neonatal infection.
I have divided the treatments in three types. Those of the first type are based on the use of chemical drugs, those of the second type are based on the use of the natural and alternative medicine and the treatments of the third type combine the use of chemical drugs and natural and alternative medicine. In this context I analyze the only treatment that eliminates the virus totally.
| What section do you want to read initially? Click on index |
| Human herpes virus infection |
| Human herpes simplex viruses |
| Oral herpes |
| Genital herpes |
| Treatments for herpes |
| Transmision of human herpes virus |
| Herpes symptoms |
| Neonatal herpes |
Human herpes virus infection [↑]
Herpes is a common viral infection. There are many different “herpes” viruses including conditions such as genital herpes, cold sores, chickenpox and shingles. Other human members of this group of viruses include Epstein-Barr virus, Human Cytomegalovirus, and the most recently discovered human herpes virus: Herpes Virus 8 that causes Kaposi’s sarcoma. The herpes viruses are also widespread throughout the animal kingdom.
The usual incubation period of the virus before any symptoms show is approximately two to twelve days after the first exposure to the virus. However, the virus can lay dormant for periods of time before any symptoms begin to show. Some people may not experience a recognizable outbreak for several months or even years after exposure.
Symptoms vary greatly from person to person. Many people never experience active symptoms (asymptomatic carriers). Symptoms vary from very mild to severe in others.
Herpes is estimated to affect about 80 million people in America. At least one in five adults in the United States has genital herpes.
Human herpes simplex viruses [↑]
Understanding the two different types of the human herpes simplex virus (HSV) is an important part of understanding herpes and its role in our society. Many people think there is a “good” human herpes virus, oral herpes, and a “bad” human herpes virus, genital herpes, partly because they don’t understand the similarities between HSV-1 and HSV-2. From a social point of view, the problem is not the disease; it’s how you got it. There is a social prejudice against genital herpes, no matter which virus causes it.
Herpes simplex viruses include two distinct but closely related viruses, namely, HSV-1 and HSV-2. Under a microscope the two viruses are virtually identical; a laboratory analysis is necessary to differentiate one of another. Both infect the body’s mucosal surfaces, usually the mouth or genitals, and then establish latency in the nervous system. Both can recur and spread even when no symptoms are present.
Oral herpes can be caused by herpes simplex virus type 1 (HSV-1) or herpes simplex virus type 2 (HSV-2), but typically, HSV-1 is above the waist. Genital herpes is usually caused by HSV-2, and generally below the waist. However it is important to note that either type can be found above or below the waist since transmission is through direct contact. HSV-1 can be transmitted from mouth to mouth through a kiss or from mouth to genitalia through oral sex. Similarly, HSV-2 can be transmitted from genitalia to genitalia through vaginal or anal intercourse or from genitalia to mouth through oral sex.
Many of the approximately 100 million Americans who are infected with oral HSV-1 acquired the virus when they were children. Usually the first herpes simplex virus that people encounter is spread simply by the kind of social kiss that a relative gives a child. Almost all of the approximately 40 million Americans infected with HSV-2 acquired the virus as teenagers or adults when they became sexually active.
About 50% of Americans have HSV-1 antibodies in their blood by the time they are teenagers or young adults. 80-90% of Americans have HSV-1 antibodies by the time they are over age 50. An HSV infection causes the body to produce antibodies, some of which are active against both HSV-1 and 2. This acquired immune response gives some limited protection if the body encounters a second type of HSV. People who have a prior HSV-1 infection have an acquired immune response that lowers the risk of acquiring HSV-2. There is evidence this acquired immune response can help reduce the acquisition of subsequent HSV-2 infection by 40%.
Oral herpes [↑]
Oral herpes, also commonly known as cold sores, fever blisters, or herpes labialis, are caused from the herpes simplex virus. The lesions are small, painful, fluid-filled blisters or sores. Cold sores are very common. It is estimated that 80% of the population have been exposed to the herpes simplex virus, HSV-1.
Oral herpes can infect the tongue. Herpes on tongue is very annoying and difficult to treat.
Cold sores are usually found on or the at the edge of the mouth or lip; or on the face near the mouth such as the chin, nose, throat, or cheek.
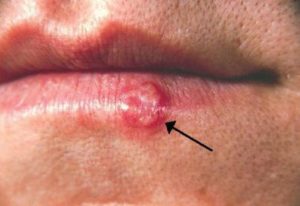
Real image of cold sores.
Once infected with cold sores, the virus remains inside the body forever, usually in a latent (dormant) state. The virus can become “activated” causing a cold sore recurrence due to many factors. An infection recurs when the virus is activated in the ganglia and travels down the nerve to the surface of the skin where it replicates. When cold sores reoccur they will typically appear in the same location that they did during previous outbreaks.
A cold sore goes through a cycle of phases typically as follows:
Prodrome: tingling and itching prior to visual outbreak; warning symptoms that last less than 6 hours.
Inflammation: swelling and redness at the site before outbreak; indication that the virus and antibodies have arrived.
Vesicular: blisters that appear within 1-2 days after prodrome from one or several vesicles, or tiny red bumps commonly found at the vermilion border of the lip.
Ulcers: actual sores that form within 3 days after prodrome, often accompanied by pain; blisters leak fluid.
Crusts: sores dry and form scabs within 4 days to indicate healing; virus diminishes and wounds heal within 2-3 days.
Healing: complete within 8-10 days; new skin forms; virus replication is complete. Virus retreats to the host ganglia where it remains protected from the host’s immunological attack.
Genital herpes [↑]
Genital herpes is a STD that is generally spread by skin-to-skin contact. It is a contagious viral infection primarily affecting the genitalia of men and women. Genital herpes may be caused by HSV-1 or HSV-2, however, is mostly caused by HSV-2. HSV-1 (or cold sores) can be transferred to the genitals and HSV-2 (or genital herpes) can be transferred to the mouth through oral sex.
Genital herpes is extremely common. In America an estimated one out of five adults are infected, but only about a third of those are aware that they have the virus. Many have either no symptoms or very mild symptoms and therefore do not relate the symptoms to herpes.
Treatments for herpes [↑]
Is there a herpes cure? In this section I am going to offer an answer to this question by analysing the available treatments.
Treatments for herpes, according to the remedy that we use, can be divided in three types. The first type contains the treatments based on the use of chemical drugs, the second type includes the treatments based on the natural and alternative medicine and the third type groups combined both treatments, that is to say, those that use chemical drugs and the natural and alternative medicine.
The treatment of the first type more suitable for the doctors is the one based on the use of Acyclovir. This drug was discovered by Howard Schaeffer in 1974 and it began to take place for its commercialization in 1984. Acyclovir acts inhibiting the synthesis of the viral DNA hindering the replication of the virus, it doesn’t eliminate the virus from our body, but it fights the symptoms of the illness and it reduces the time of the outbreaks.
The price of Acyclovir varies from a country and another, but because the herpes is recurrent, it can be expensive in the long term. Acyclovir is marketed with different presentations: pills, injections, suspensions for the use of children, creams and ointments.
The topical use of Acyclovir has not frequent noxious side effects and light. Its oral use has more frequent adverse effects: headache, nauseas, vomits, abdominal pain and diarrheas. Its intravenous use can cause hematuria (presence of blood in the urine), hypotension and encephalopathy (brain disease).
The use of Acyclovir is contraindicated for: 1) dehydrated patients, 2) patients with alterations in the renal functions, 3) pregnant women and 4) women in period of nursing.
Treatments for herpes of the second type, that is to say, those based on the natural and alternative medicine are varied. This type includes home remedies, use of medicinal herbs, use of devices using light, use of creams and natural oils, acupuncture and use of patches. These treatments don’t eliminate the virus from our body and some of them are expensive.
The combined treatments have arisen in different variants. Some of them have demonstrated to be very effective to fight the virus and outbreaks. The Ultimate Herpes Protocol is the combined treatment of better results. It was created by a doctor and British researcher to kill herpes virus.
The Ultimate Herpes Protocol was exposed in a book written originally in English language and it has been translated to other languages. You can download it in English from its official website. You can download it in Spanish by clicking on this link.
| Table 1: Treatments for herpes | ||||
|---|---|---|---|---|
| Type of treament | Example | Remedies | Noxious side effects | Effects against virus |
| Based the use of chemical drugs. | Treatment with Acyclovir. | Acyclovir, Valacyclovir and Famciclovir. | Noxious side effects in oral and intravenous forms. | It impedes replication of virus, but it doesn’t eliminate virus. |
| Based the use of natural and alternative medicine. | Tea Tree Ointment | Natural creams and oils, medicinal herbs, acupuncture, patches and devices using light. | Without noxious side effects. | It avoids the appearance of outbreaks and reduces their permanency, but doesn’t eliminate virus. |
| Combined treatments. | The Ultimate Herpes Protocol (UHP). | Natural remedies and drugs without noxious side effects. | Without noxious side effects. | It impedes the outbreaks or reduces their time of permanency. UHP elimine virus. |
Transmission of human herpes virus [↑]
Human herpes virus can spread from person to person by direct contact, that is, directly from the area of infection to the area of contact, unlike a flu virus that you can get through the air. Herpes is most easily spread when a sore is present, but, one does not have to have symptoms in order to be contagious. Due to a phenomenon known as Viral Shedding, the virus can be spread from contact with the apparently normal skin of an asymptomatic carrier, so it is possible for a person to transmit the infection to their partner without even knowing they are infected.
An infected person can spread the virus to other parts of his or her own body. The fingers, eyes, and other body areas can accidentally become infected by self-inoculation and contamination by touching the location of an outbreak or viral shedding and then touching, rubbing or scratching another part of the body.
Cold sores can be caused by HSV- 1 or HSV-2, but typically, HSV-1 is above the waist. Genital herpes is usually caused by HSV-2, and generally below the waist. However it is important to note that either type can be found above or below the waist since transmission is through direct contact. HSV-1 can be transmitted from mouth to mouth through a kiss or from mouth to genitalia through oral sex. Similarly, HSV-2 can be transmitted from genitalia to genitalia through vaginal or anal intercourse or from genitalia to mouth through oral sex.
Transmission of oral herpes
The virus is spread from person to person by skin to skin contact with an infected area. Kissing someone with a lesion is a very common way for the virus to be transmitted. One does not have to have symptoms in order to be contagious. Due to viral shedding, the virus can be spread due to contact with the apparently normal skin of an asymptomatic carrier. Infected saliva may also be a way of transmitting the virus. It also may be possible to transmit the virus particles through objects such as a drinking glass, eating utensil, lipstick, lip gloss, toothbrush, or even a face cloth.
Transmission of genital herpes
The virus is spread from person to person by skin to skin contact with an infected area, not through the air like a flu virus. Intercourse, oral or anal sex, masturbation, and rubbing against the infected area are common examples of how the virus can be transferred. One does not have to have symptoms in order to be contagious. Due to viral shedding, the virus can be spread due to contact with the apparently normal skin of an asymptomatic carrier.
An uninfected individual has about a 75% chance of contracting the illness during intimate contact with someone actively shedding virus. However, since asymptomatic viral shedding occurs without any signs or symptoms, it is impossible to know exactly when viral shedding is happening.
The human herpes virus does not pass through latex condoms. Condoms do not provide 100% protection because there could be a lesion which the condom did not cover. It is important to remember that the virus can be spread when a person has no symptoms through viral shedding. Therefore condoms or latex barrier protection should also be used between outbreaks for additional protection. When used consistently condoms are one of the best available forms of prevention.
Herpes symptoms [↑]
Symptoms of herpes usually develop two to twelve days after the first exposure to the virus, but it could take longer. The virus can lay dormant and may be in your system for years before any symptoms show. Some people never experience active symptoms. For these reasons many people infected with HSV are not aware of their infection.
We know the duration of symptoms varies from one person to the next and may last up to several weeks.
The first outbreak is normally the worst. The symptoms during a first outbreak can be quite pronounced. However, sometimes the first infection is so mild it may go unnoticed.
The virus multiplies when it gets into the skin cells. Our skin becomes red and sensitive, and shortly after blisters or bumps appear. The blisters first open, and then heal as new skin tissue forms. The active phase of infection is over when the sores are completely healed. There is usually no scarring. When the active phase is over, the virus retreats into the nervous system in a latent (dormant) state. A person may or may not experience a subsequent recurrent outbreak. If a recurrence does happen it often corresponds with a weakened immune system due to stress, illness, medications, etc. Sun exposure is often a ‘trigger’ for a recurrence of cold sores.
Cold sores symptoms
Before a cold sore appears one may experience symptoms such as pain, itching, or tingling. This is called the prodromal stage of the outbreak, which often precedes the blisters by one to two days.
Cold sores typically appear as small, fluid-filled blisters. The blister will usually ulcerate (seep) and then form a scab before healing and disappearing completely. A typical cold sore outbreak lasts from 8 to 12 days.
Genital herpes symptoms
If the infection is located in the genital area a number of symptoms may be experienced. The area is usually painful and there may be itching, tingling, or burning sensations; a blister, cut, tear, sore, bump or rash; muscle aches or pains near to the area; burning and/or pain when urinating; and vaginal or penile discharge. It is also common for flu-like symptoms such as headache, fever and swollen glands to accompany an initial outbreak of genital herpes.
Shingles symptoms
Shingles starts as a rash of small blisters on a red base, with new blisters continuing to form for three to five days. The rash typically appears on one side of the body, the left or right, in a band, a strip, or area that follows the path of individual nerves that come out of the spinal cord. Shingles is most common on the trunk and buttocks. But it can also appear on the face, arms or legs. Up to one week before the rash appears a person may experience a burning pain or sensitive skin. On occasion, the pain will be present but the blisters may never appear. Eventually, the blisters pop and seep. The affected areas will then crust over and heal. The outbreak may last three to four weeks from start to finish.
Many people who experience a shingles outbreak find it extremely painful. The acutely painful phase usually lasts several weeks but some people continue to have pain long after the outbreak has cleared. This is known as post-herpetic neuralgia and it is the most common complication of shingles. Post-herpetic neuralgia can be severe and debilitating. It occurs primarily in people over the age of 50.
Neonatal herpes [↑]
A potentially serious complication can arise when a mother has been infected with the virus, neonatal herpes. Since a baby’s immune responses are not developed as with an adult, this is a very severe and potentially fatal condition. Babies can become infected during the pregnancy or during birth when passing through the birth canal. If a baby is born with herpes it can develop serious problems that may affect the brain, skin or eyes. Half of the babies infected with herpes will die or have nerve damage.
The risk of the baby being infected during delivery is much lower if a woman has a genital herpes outbreak during pregnancy that is not an initial outbreak. If a woman has her first outbreak of genital herpes while she is pregnant, she can pass the virus to her unborn child and may deliver a premature baby. Pregnant women who are infected with genital herpes should stay in close contact with their physician or healthcare provider before, during and after the pregnancy.
If there are active herpes lesions in or around the birth canal during labor and delivery the physician should perform a cesarean section to prevent infection of the baby. Most women who have the human herpes virus can have a normal delivery as they will most likely not have an active infection during labor and delivery.
To protect yourself and your unborn child a pregnant woman should take the appropriate precautions to prevent acquiring the virus or a recurrent outbreak. First and foremost, the immune system is a key factor in controlling outbreaks. The immune system is responsible for keeping the body healthy and fighting off pathogens like the human herpes virus. Help defend against the virus by paying attention to your body and taking simple precautions that will help boosting your immune system. Getting enough rest, moderate exercise, eating a healthy diet containing fresh fruits and vegetables, and lowering stress levels will help boosting the immune system. Here are some other steps for prevention:
- Avoid sexual intercourse during an active episode of the disease, because this is when the virus is most likely to be transmitted.
- Use latex condoms to reduce the risk of transmitting the virus between outbreaks.
- Limit the number of sexual partners.
Conclusions
I hope the reading of this article has been useful to know more about the human herpes virus, the illnesses that it can cause and the treatments to use to fight them.
Articles to broaden your knowledge:
https://medlineplus.gov/druginfo/meds/a681045.html (You can find more information about acyclovir in this article).
I like the helpful info you provide in your articles.
I'll bookmark your weblog and check again here regularly.
I'm quite certain I'll learn lots of new stuff right here!
Best of luck for the next!